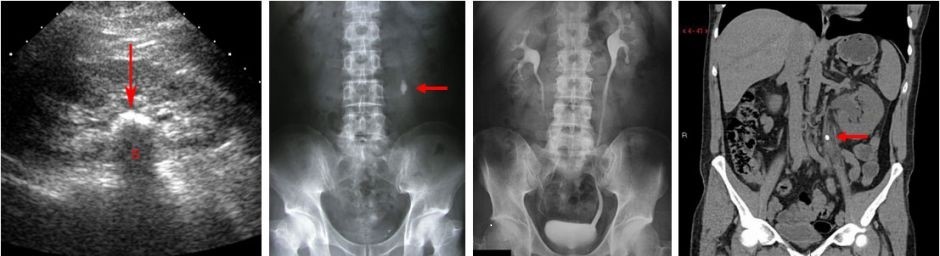
Lithiasis

|
|
|
|
|
||||||||||
|
How is the diagnosis made? The diagnosis of lithiasis is made by the history, the clinical examination and the necessary laboratory and imaging tests. The history and clinical examination raise the suspicion of lithiasis to the urologist, and the diagnostic tests are aimed at confirming the diagnosis, investigating the functionality and morphology of the urinary system, and detecting possible etiological factors responsible for the formation of stones. The tests used to investigate lithiasis are divided into imaging and laboratory tests. If you need to do some of these, your doctor will recommend it. |
|
|
|
Laboratory check: - General urine: Usually, there are red blood cells in the urine and sometimes evidence of a urinary tract infection. How is lithiasis treated? Treatment of symptoms In a small percentage of patients, some immediate intervention will be needed when: In these cases, a ureteral catheter (pig-tail) may need to be inserted. Through the urethra with endoscopic instruments, the doctor reaches the bladder, finds the opening of the ureter and through it advances the catheter to the kidney. In cases where this is not possible, the tube is placed through the skin (percutaneous nephrostomy). If the conditions allow it, the removal of the stone can be done at the same time.
In some forms of stones, your doctor can prescribe you medicines, which aim either to reduce the size of the stone or to prevent its re-formation. Medicines differ depending on the chemical composition of the stone and whether there is any metabolic disease. |
|
||||||||||
|
What is the necessary follow-up afterwards? The probability of new stone formation one year after the initial stone episode is 10%, with the percentage increasing to 30-40% after 5 years and 50-60% in ten years. Therefore, it is necessary to monitor patients with lithiasis individually, depending on the individual's predisposition to create stones at intervals, which will be determined by the attending physician with a kidney-bladder ultrasound and plain X-ray of the kidneys, ureters and bladder (NIC). Furthermore, it is necessary to take measures to avoid the recurrence of lithiasis. Your urologist will recommend that you: Make sure you drink 2 to 2.5 liters every day |